As Lieutenant in Navy Reserve, Georgetown BSN Alumna Cares for Patients with COVID-19
May 1, 2020 – Jen Tran (NHS’11), a BSN alumna, is about to mark eight years in the U.S. Navy Reserve, where she is currently a lieutenant. Since early April, she has been helping care for patients with COVID-19 in New York City.
“The mission in New York City is very unique, where different units and detachments from our military forces have come together to help combat the pandemic,” she said. “Our military medical staff have been present on the USNS Comfort, in the Javits Convention Center, and across many of the New York City hospitals to help augment and support the staff and patients.”
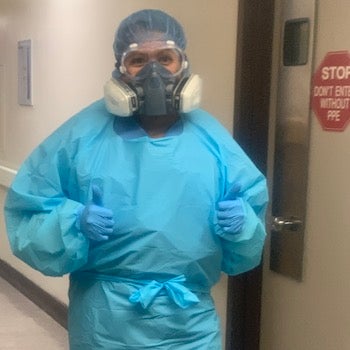
Tran, who was commissioned as an officer approximately a year following her Georgetown graduation, is now serving as a critical care nurse in a Bronx hospital.
“It’s hard to work the front lines and seeing firsthand the worst case scenarios of COVID-19,” she said. “The impact this virus has had on any community will be forever felt in every way.”
Global Service
In her civilian life, Tran is a nurse practitioner in the gynecologic oncology division at Baptist MD Anderson Cancer Center in Jacksonville, Florida.
Before this current Navy deployment in New York City, Tran was deployed six years ago in the Middle East, serving as a critical care nurse for the Expeditionary Resuscitative Surgical System.
Also in 2014, with a non-governmental organization, she traveled to Lunsar, Sierra Leone, where she treated patients with Ebola.
“Going into this fight, I thought to myself, ‘if I survived Ebola, then I can do coronavirus,’” Tran said, remembering how hot it was wearing personal protective equipment (PPE) in Sierra Leone.
“PPE still stands at a critical shortages pretty much everywhere, but supplies are being delivered and cautiously distributed so each team member can be protected safely,” Tran added. “There is always a worry that there won’t be enough PPE, but luckily we haven’t had that situation for our team yet.”
‘A Full Grasp of the Disease’
Tran said she has learned a great deal about COVID-19 during her deployment.
“Before coming to New York City, I don’t believe I had a full grasp of the disease and the disease process, based on reports and articles I had read or listened to,” she said. “Seeing it firsthand and working in the intensive care unit, I was extremely shocked by the impact on each and every single patient.”
COVID-19 impacts respiratory function for many patients, Tran said. Yet for critically ill ones, the virus “displays as a multi-organ dysfunction syndrome, some ways in which I have never seen manifest before,” she added.

Many patients have been taking multiple medications focused on different aspects of the body, she said.
“For any nurse, the management of these drips and mechanical ventilation can be stressful, but even more so for nurses with minimal ICU experience,” she said. “We’re lucky to have lifesaving resources and technology to mitigate worsening disease; however, many of the patients I have cared for have passed, and those who have survived will have lifelong health issues.”
Care and Compassion
Tran said her education at Georgetown has been influential in her career in professional and advanced practice nursing.
“My studies at Georgetown have truly shaped my approach and thinking to caring for a patient, and I believe I am the best nurse and nurse practitioner because of that,” she said. “I had the opportunity to take elective courses during my undergraduate studies focusing on death and dying, palliative care, and also bioethics.”
She said this has helped prepare her for hard conversations about end-of-life care.
“As a nurse, I feel that I am able to bridge the gap between provider and patient, but also help educate others on this,” Tran added. “Communication has been key, especially as patients and families are unable to be together during this crisis at the hospitals. We are using iPads to help with video calls so families can see and talk with their loved ones.”
Tran said she has experienced powerful moments of connection with her patients in this time of isolation.
“As patients are alone, I feel that the sense of touch can be so powerful in such a somber situation,” she said. “I have frequently held my patients hand, wiped tears from their eyes when they don’t have the strength to, comforted patients with words – all things of providing compassionate care and cura personalis. . . . I always put my patients first and provide the utmost and best care for them, giving them 110 percent of what I have.”
- Tagged
- COVID-19
