Georgetown BSN Alumna Works on COVID-19 Response at Dallas Hospital
April 15, 2020 – Mary Catherine Keckeisen (NHS’18), who earned her BSN at Georgetown, regularly serves as a critical care nurse in the medical intensive care unit (MICU) at Parkland, a hospital in Dallas.
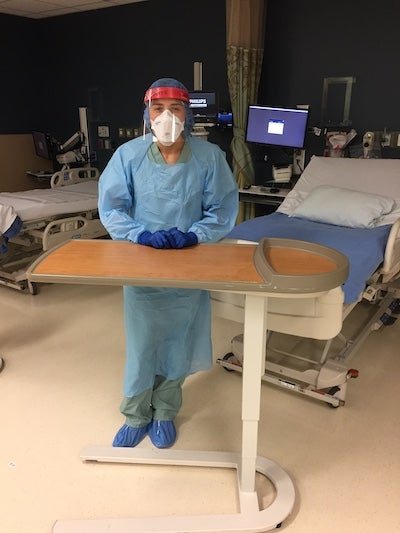
Late last month, given an increase in patients with COVID-19, she volunteered to work on the hospital’s tactical care unit (TCU), “a floor of the hospital repurposed into a giant ward for coronavirus patients.”
“It was definitely an adjustment at first,” Keckeisen said. “Every staff member has to remain in an N95, face shield, gown, and gloves at all times unless at lunch.”
‘Never Loved Nursing More’
The patients Keckeisen helps care for on the TCU “are extremely sick,” and the days are long and hot, given the clinical attire. Due to increasingly limited supplies, she added, the health providers are no longer receiving new N95 respirator masks on a daily basis.
“But even with all the cons, I have never loved nursing more,” she said. “I feel called to be working on the TCU, and my work feels meaningful.”
Keckeisen said this experience differs from the patients she usually works with in the MICU, most of whom “have an extensive list of comorbidities.” She added, “After coming through the unit, many end up in nursing homes or long-term care facilities.”
“In the TCU, however, my patients have few – if not no – comorbidities,” she said. “These people are often otherwise healthy. It’s extremely humbling to see how life can turn on a dime. Yet it’s also been wonderful to see the recoveries, as these are patients who are, for the most part, otherwise healthy. When these patients are treated well, they can heal. They can go home to live not one or two years, but a lifetime. There is a stark dichotomy between the patients I saw two months ago and the patients I’m seeing now.”
‘Go Where I Am Needed’
Keckeisen said the lessons she learned at Georgetown have helped guide her during the first years of her career in nursing.
“Georgetown taught me that I should always be open to flexibility in my nursing career and go where I am needed,” she said. “Having professors who had worked in every field within nursing made me realize that the profession of nursing is just a big, beautiful umbrella. We can and do go where we are needed.”
Keckeisen remembered hearing a guest lecture in one of her undergraduate courses that featured a public health nurse who worked on the Ebola response in Africa.
“Even though this nurse hadn’t worked at the bedside for over a year, she was still able to care for patients after learning what she needed to on the job,” she said. “That stuck with me. I never wanted to turn down an opportunity to help out in a disaster.”
Supportive Team
About her team, Keckeisen said: “The collaboration at Parkland has been phenomenal.”
“Unlike many cities, Dallas has had quite a bit of time to prepare for our ‘peak,’ so our hospital administrators, doctors, and nurse managers worked together to streamline the creation of a new unit,” she said. “In this unit, nearly everyone has taken on new responsibilities or roles.”
The teamwork has allowed her to interact with and learn from nurses and surgical technologists across units.
“We use mobile computers with video conferencing so entire teams of doctors can round on the patients without using PPE, though there is always one attending physically on the unit,” she said. “In addition, the layout of the ICU itself is optimal for collaboration as it’s a large room in which only curtains separate the patients from the providers.”
Said Keckeisen: “Everyone has stepped up to the plate to battle this pandemic.”
- Tagged
- COVID-19
